✍️ Written by: LSRI Editorial Team
🩺 Medically Reviewed by: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
📅 Last Updated: April 1, 2026
⏱️ Read Time: 5 Minutes
Raynaud’s phenomenon can be incredibly painful and disruptive, especially when attacks are frequent, prolonged, or complicated by digital ulcers that struggle to heal. For patients with severe, non-responsive symptoms, understanding how botox for Raynaud’s phenomenon works can provide a new pathway for relief. At London Sports and Rheumatology Imaging (LSRI), we see many patients who have exhausted traditional vasodilator therapies and are looking for advanced clinical options to manage their condition and prevent tissue damage.
Standard treatments such as lifestyle strategies and vasodilator medications are helpful for many people, but a significant minority continue to have severe symptoms, which has driven interest in newer clinical options such as botulinum toxin (Botox) injections. In this article, we look at the latest evidence, what the research actually shows, and who might be considered for this off‑label treatment in specialist London centres.
This article is designed as general education only and is not a substitute for a personalised assessment with your GP, rheumatologist or vascular specialist.
What is Raynaud’s phenomenon?
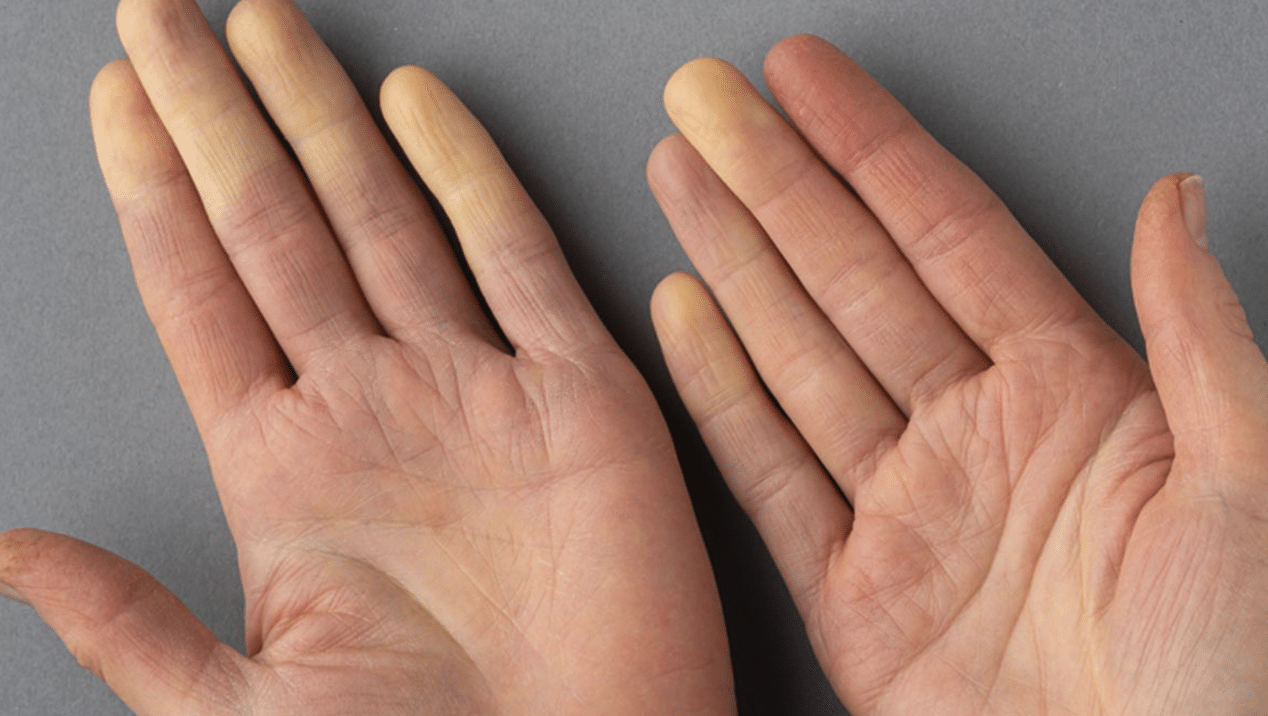
Raynaud’s phenomenon is a condition in which the small blood vessels in the fingers and toes go into spasm (vasospasm), usually in response to cold or emotional stress. This overreaction of the sympathetic nervous system causes the vessels to constrict tightly, leading to the characteristic color changes of white (ischaemia), blue (hypoxia), and red (rubor) as the blood returns. These episodes are often accompanied by numbness, intense pain, and a throbbing sensation as the ‘re-warming’ phase begins.
Raynaud’s can occur in two forms:
- Primary Raynaud’s: This is the most common form and occurs on its own without an underlying disease. While uncomfortable, it is rarely progressive.
- Secondary Raynaud’s: This is associated with an underlying autoimmune condition like systemic sclerosis (scleroderma) or lupus. In secondary cases, the lack of blood flow can be severe enough to cause skin breakdown, resulting in chronic, painful digital ulcers and, in extreme cases, gangrene.
Standard treatments – and where Botox fits in
First‑line management for most people focuses on lifestyle and trigger avoidance: keeping the whole body warm, layering clothing, and managing stress. When symptoms remain problematic, medications such as calcium‑channel blockers (e.g., nifedipine or amlodipine) are commonly prescribed. These drugs work systemically to dilate blood vessels across the body.
However, a significant portion of patients do not tolerate these medications due to side effects like headaches, lightheadedness, or ankle swelling. Furthermore, in cases of severe secondary Raynaud’s, oral medications may not provide sufficient local blood flow to heal existing ulcers. This is where botox for Raynaud’s phenomenon emerges as a targeted, local intervention typically reserved for those who have not responded adequately to standard therapies.
How Botox for Raynaud’s Phenomenon improves circulation
Botulinum toxin works by temporarily blocking the release of acetylcholine and other chemical messengers at nerve endings, which effectively relaxes the smooth muscles surrounding the digital arteries. This creates a “chemical sympathectomy,” reducing the intensity of vasospasms and allowing more blood to reach the fingertips. Several clinical studies suggest that botulinum toxin can increase skin temperature, improve capillary flow, and significantly reduce the time it takes for hands to recover after a cold challenge.
Latest Evidence on Botox for Raynaud’s Phenomenon
The clinical evidence for botulinum toxin has grown significantly in recent years. A 2024 systematic review and meta-analysis of 13 studies (286 patients) demonstrated that botulinum toxin therapy was associated with:
- Statistically significant pain relief: A marked reduction in Visual Analogue Scale (VAS) pain scores.
- Functional improvement: Better scores in the Disabilities of the Arm, Shoulder and Hand (QuickDASH) questionnaire.
- Ulcer healing: Accelerated healing in patients with chronic digital ulcers secondary to scleroderma.
While these results are promising, it is important to note that most studies are small, and larger randomised controlled trials (RCTs) are currently underway to further define optimal dosing and injection patterns.
Internal links: Explore more on our blog or contact us for a consultation.
Who might (and might not) be considered for Botox?
Potentially suitable candidates in specialist practice typically include those who:
- Have severe, frequent Raynaud’s attacks that significantly interfere with work or daily living.
- Have non-healing or recurrent digital ulcers despite being on multiple vasodilators.
- Are under the care of a specialist rheumatology or vascular team.
Safety and side effects
Across published literature, serious complications are rare. The most frequently reported side effect is temporary hand weakness (intrinsic muscle weakness), which can affect fine motor tasks for a few weeks but is usually self-limiting. Bruising at the injection site is also possible. Because it is used ‘off-label’ for this condition, it is vital that the procedure is performed by an experienced specialist who can precisely target the digital arteries while avoiding major motor nerves.
FAQs about Botox for Raynaud’s

About the Author: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
Dr Prashant Sankaye is a highly respected Consultant MSK Radiologist and the Clinical Director of London Sports & Rheumatology Imaging (LSRI). With over a decade of sub-specialty experience, he is a recognized expert in advanced diagnostic imaging (Ultrasound & 3T MRI) and precision ultrasound-guided therapeutic injections. His authoritative approach ensures patients avoid surgery where possible and receive the highest standard of orthopaedic, rheumatological, and sports medicine care.