✍️ Written by: LSRI Editorial Team
🩺 Medically Reviewed by: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
📅 Last Updated: March 30, 2026
⏱️ Read Time: 5 Minutes
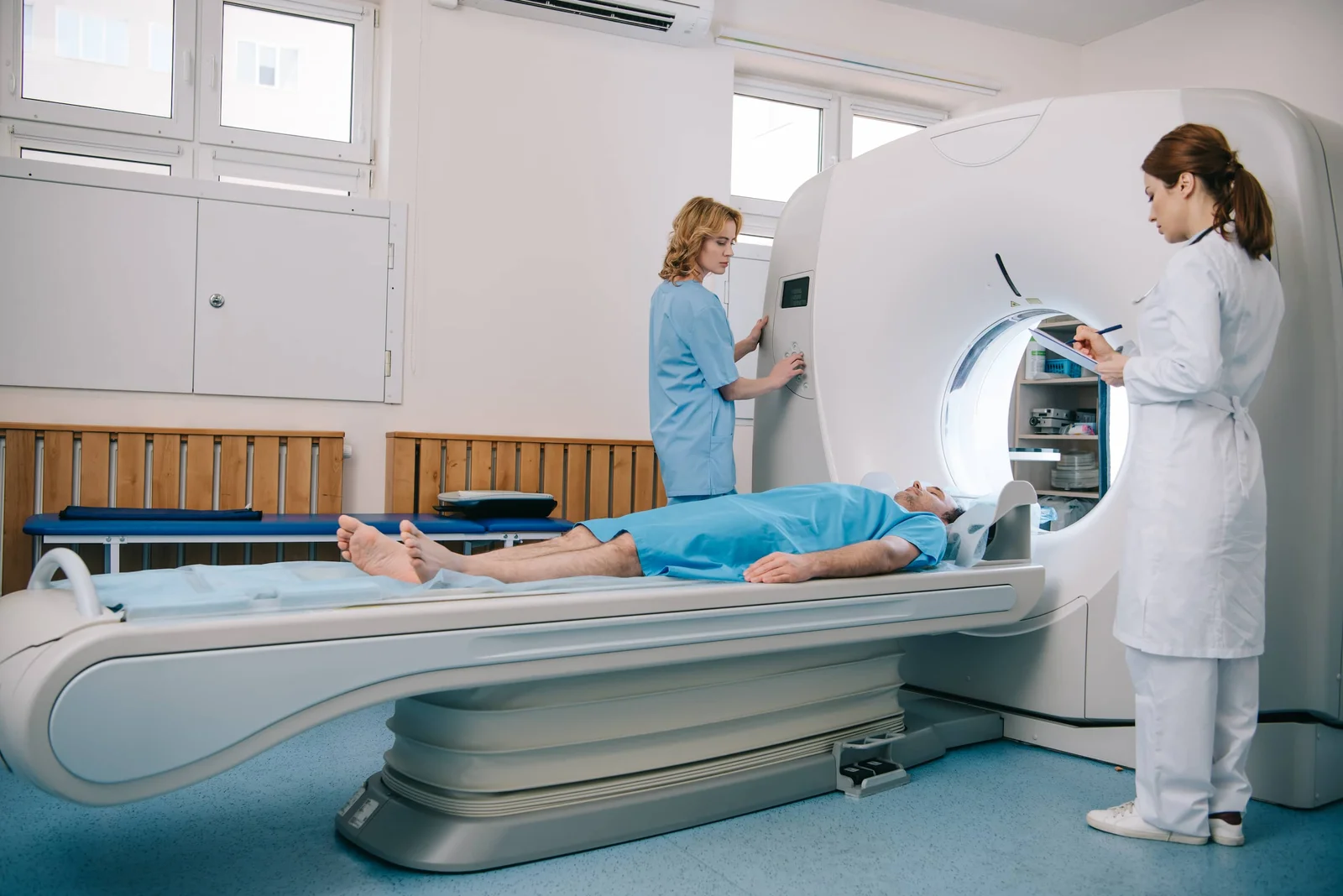
When it comes to Early Imaging, an accurate diagnosis is the first and most critical step toward effective treatment. At LSRI London, we specialize in high-resolution imaging to ensure you receive the precise care your joints need.
Too many patients with musculoskeletal pain are still being pushed into weeks or months of treatment before anyone has properly established what is actually wrong. That is the central problem. When pain, locking, swelling, weakness, tendon injury or joint instability are treated without clear imaging, patients can lose time, lose money, and in some cases lose the chance for earlier, more effective treatment.
Dr Prashant Sankaye, whose professional profiles describe him as a sports injury, musculoskeletal and spine radiologist, is positioned around precisely this point: diagnosis should guide treatment, not the other way around. At London Sports and Rheumatology Imaging, patient reviews repeatedly emphasise prompt diagnosis, clear explanations and guidance on next steps, reflecting our clinic’s 5.0 Google rating.
Not every minor ache needs an immediate MRI. But many patients with persistent symptoms, failed rehabilitation, recurrent swelling, mechanical locking, post-traumatic pain, or major weakness should not be left in a vague “let’s try a few more sessions and see” pathway. That delay can be clinically costly and emotionally exhausting.
The Problem with Delayed Diagnosis
A surprising number of musculoskeletal complaints are still approached backwards. A patient develops knee pain, shoulder pain, Achilles pain or back-related limb symptoms, and the first step becomes a package of exercises, manipulation, stretching, or repeated hands-on treatment without any certainty about whether there is a structural tear, meniscal displacement, tendon rupture, cyst, stress injury, inflammatory change, or another diagnosis altogether.
This is where patients are often told that conservative treatment is automatically the cheaper and wiser option. In reality, it can become the classic “penny wise and pound foolish” decision. Paying for several sessions of treatment that do not address the true pathology is not efficient care. It is delayed care.
The modern standard should be more intelligent than that. Good medicine is not about doing more treatment first. It is about understanding the problem first. Once the anatomy and pathology are defined, the patient can move into the right pathway with far greater confidence — whether that means physiotherapy, injection therapy, load modification, orthopaedic referral, rheumatology input, or reassurance.
Why Imaging Changes the Pathway
Imaging is valuable because it reduces guesswork. A proper MRI or targeted ultrasound can reveal whether pain is coming from a meniscal tear, tendon degeneration, tendon rupture, ligament injury, cartilage damage, bursitis, synovitis, cyst formation, bone stress response, or another structural problem that is simply not obvious from symptoms alone.
That matters because different injuries need completely different advice. Some problems improve with a structured rehabilitation programme. Some require temporary unloading. Some need image-guided injection. Some need surgical opinion. Some need urgent escalation because continuing aggressive treatment risks worsening the damage.
This is also why early imaging is not anti-physiotherapy. Quite the opposite. The best rehabilitation happens when physiotherapy is based on facts. Imaging can help good therapists target the correct tissue, avoid unsafe loading, and stop treating the wrong diagnosis.
Case Study: The Locked Knee That Needed Clarity
One notable example is a recent football-related knee injury encountered at LSRI. A patient presented with ongoing medial knee pain, intermittent posterior pain, significant swelling linked to recent flare-ups, and episodes of joint locking. Despite three full months of physiotherapy, they experienced only partial (50-60%) recovery. Their pain worsened predictably with deep squats and high repetitions, and they even required a brace for long-distance walking.
That sort of clinical presentation should always make clinicians pause. Mechanical symptoms like locking and failure to recover after several months are red flags pointing strongly toward a structural problem. Initially, the patient was dealing with what was suspected to be a simple medial meniscus tear.
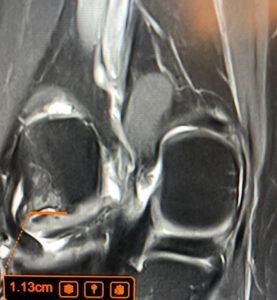
In this case, an expert 3T MRI interpretation changed the understanding completely: instead of a simple incomplete recovery from a minor tear, the high-resolution scan identified a complex bucket-handle type tear displaced into the intercondylar notch, along with a small parameniscal cyst. The whole story and treatment protocol changes instantly once that specific anatomical reality becomes visible.
The lesson is clear. If a patient has ongoing locking, swelling, weakness, or persistent pain after months of treatment, there has to be a lower threshold for imaging. Continuing the same plan without an accurate diagnosis is not persistence. It is clinical drift.
Other Patterns Seen Again and Again
The same diagnostic delay frequently occurs in shoulder problems. A patient may be told they have “frozen shoulder” and spend weeks stretching into pain, when the real issue is a substantial rotator cuff tear, severe bursitis, or a different pathology that should have been imaged before aggressive rehabilitation was prescribed.
It also happens in tendon injuries. A patient with chronic Achilles pain may be placed into a standard loading programme, even though the tendon may already have advanced degeneration or partial tearing. Without high-resolution imaging, the treatment may sound reasonable but still be wrong for that specific tendon on that specific day.
Patients deserve better than protocol-driven guesswork. They deserve a pathway built around what is actually inside the joint, tendon or soft tissue.
What Patients Should Know Now
If you have persistent musculoskeletal pain, failed physiotherapy, recurrent swelling, reduced strength, instability, locking, or a sports injury that is not progressing as expected, it is entirely reasonable to ask whether imaging should happen sooner rather than later. That is not being difficult. It is being informed.
At LSRI, the message is simple and modern: diagnose first, then direct treatment properly. Early imaging does not mean every patient needs an MRI immediately. It means patients with meaningful symptoms should not be left wasting months in clinical uncertainty when modern imaging can provide clarity, direction and, in many cases, a much better plan.


About the Author: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
Dr Prashant Sankaye is a highly respected Consultant MSK Radiologist and the Clinical Director of London Sports & Rheumatology Imaging (LSRI). With over a decade of sub-specialty experience, he is a recognized expert in advanced diagnostic imaging (Ultrasound & 3T MRI) and precision ultrasound-guided therapeutic injections. His authoritative approach ensures patients avoid surgery where possible and receive the highest standard of orthopaedic, rheumatological, and sports medicine care.