✍️ Written by: LSRI Editorial Team
🩺 Medically Reviewed by: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
📅 Last Updated: April 18, 2026
⏱️ Read Time: 16 Minutes
The delayed diagnosis elbow tumour case presented here illustrates the critical importance of early and accurate imaging. Accurate diagnosis of an elbow tumour is critical, as shown in this case where a year of pain was initially misattributed.
Last medically reviewed: April 2026 by Dr Prashant Sankaye FRCR, Consultant Musculoskeletal, Spine and Sports Radiologist.
A sore elbow. A referral to physiotherapy. Some anti-inflammatory tablets. More physiotherapy. A different physiotherapist. Another referral.
Sound familiar? For thousands of patients across the UK every year, persistent limb pain follows exactly this path – round and round a loop of well-intentioned but ultimately misdirected treatment – while the real cause sits undiagnosed, sometimes growing, sometimes spreading, always waiting.
The MRI image below tells one such story. After one year of elbow pain, a patient was finally referred for MRI. What it showed was not a soft-tissue injury, not a tendon problem, not anything that a year of physiotherapy could ever have helped.
It showed a tumour.
This article is not a criticism of physiotherapists or GPs – they are skilled professionals working under enormous pressure. It is a call to action: for patients, for referring clinicians, and for a healthcare system that must understand that diagnosis shouldn’t be a question of luck until proved otherwise.
At LSRI and ScanNearMe, our ethos is simple and non-negotiable: diagnose first, treat later. Not guess first, treat later. Not refer to physiotherapy first, ask questions later.
Diagnose first.
What you are looking at in this MRI

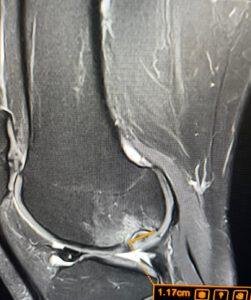
The MRI image above shows the elbow of a patient who had been experiencing persistent pain for approximately twelve months. The orange arrows point to a soft tissue mass – a tumour – that has been present throughout this period of investigation and treatment.
This was not a subtle finding. This was a measurable lesion, annotated at 7.11 cm on the sagittal sequence (left panel), with clear signal characteristics on the axial section (right panel) that distinguish it from normal surrounding tissue.
A 7-centimetre mass. One year. Undiagnosed.
Dr Prashant Sankaye reviewed this imaging as part of his specialist MSK reporting work at LSRI (lsri.uk). The finding was unambiguous on MRI – the kind of lesion that requires urgent onward referral to a bone and soft tissue tumour specialist, not a repeat course of physiotherapy.
This is not a unique case. The average diagnostic delay for soft tissue sarcoma is at least seven months longer than for other tumour types. The rarity of these tumours – combined with their ability to mimic far more common conditions such as muscle strain, tennis elbow, bursitis or tendinopathy – makes them dangerously easy to miss without imaging.
The elbow is not the most common site for musculoskeletal tumours, but bone and soft tissue tumours do occur there – and when they do, they are notoriously difficult to diagnose on clinical grounds alone.
A published review of bone tumours around the elbow found that the average delay in diagnosis can be up to two years, partly because the most common presentation – persistent, non-mechanical pain – mimics many benign conditions.
Patients may present with:
- Persistent elbow pain that does not follow a clear mechanical pattern (not better with rest, not related to a specific activity).
- Swelling or a palpable mass, which is sometimes attributed to bursitis, a ganglion or soft tissue thickening without imaging.
- Stiffness, reduced range of movement or a sensation of something “not right” that does not improve despite appropriate conservative measures.
- Night pain – a particularly important red flag that is often under-emphasised in primary care.
In many cases, patients are given a working diagnosis of lateral epicondylitis (tennis elbow), medial epicondylitis (golfer’s elbow), bursitis, a sprain or tendinopathy, and treatment begins before any imaging is obtained.
Physiotherapy for epicondylitis does not treat a tumour. Anti-inflammatory medication for presumed tendinopathy does not reduce a soft tissue sarcoma. Every week of misdirected treatment is a week in which the underlying diagnosis remains unknown and the window for less invasive intervention quietly closes.
The medico-legal and clinical literature is consistent on this point: delay in diagnosing soft tissue and bone tumours causes real, measurable harm.
Increased tumour size and stage
Studies examining highly malignant soft tissue sarcomas of the extremity with delayed diagnosis consistently show that tumours presenting late tend to be larger at diagnosis, increasing the complexity of surgery and the likelihood of requiring more aggressive resection or even amputation.
The Annals of the Royal College of Surgeons of England found that late diagnosis is considered a key reason for inferior sarcoma survival rates in England compared with Europe, with the risk of dying within one year increasing sharply as tumour stage advances – from 0% for Stage 1A tumours to 30-40% for Stage 4 disease.
The misuse of physiotherapy
This is perhaps the most important point for patients to understand: physiotherapy is not a neutral intervention when the underlying diagnosis is unknown.
A sarcoma that is repeatedly mobilised, massaged or loaded through progressive exercise will not improve. Worse, repeated consultations with physiotherapists and GPs – in which the patient is reassured and the diagnosis of “soft-tissue problem” is reinforced – make it psychologically harder for patients to push for imaging, and clinically harder for later reviewers to take the persistent symptoms seriously.
The MDU (Medical Defence Union) has published case analysis showing that in sarcoma diagnostic-delay cases, common errors include: failure to arrange appropriate imaging, failure to refer when symptoms persisted or evolved, and failure to reconsider an initial diagnosis when the patient returned repeatedly without improvement.
The financial cost
Beyond the human cost, repeated physiotherapy courses for an undiagnosed tumour represent a significant financial waste for patients who are paying privately, as well as for the NHS. A typical private physiotherapy course in the UK costs 40 to 100 pounds per session; multiple courses over twelve months can easily reach 1,000 to 3,000 pounds with no clinical benefit – while a single MRI scan, reported by a specialist musculoskeletal radiologist, could have provided the answer within days.
NICE guidance and sarcoma referral guidelines are clear about when urgent investigation and specialist referral are required.
If any of these features are present – and particularly if more than one applies – imaging should be obtained urgently. Not after another six weeks of physiotherapy. Now.
For soft tissue and bone tumours, imaging must be selected carefully and interpreted by an experienced musculoskeletal radiologist.
Plain X-ray – useful but limited
X-ray has a diagnostic accuracy of approximately 87% for bone tumours in published studies, but its sensitivity for early lesions and soft tissue involvement is much lower. Bone tumours only become visible on X-ray once they have caused sufficient cortical disruption or mineralisation – by which point the tumour may already be at an advanced stage. Soft tissue tumours are largely invisible on plain radiography.
A normal X-ray does not exclude a bone or soft tissue tumour and must never be used as the only investigation in a patient with persistent, unexplained pain and any red-flag features.
Ultrasound – first-line for soft tissue masses but has important limitations
Ultrasound is recommended by NICE as the first investigation for a suspected soft tissue mass, and can be performed within two weeks under urgent pathways. It is widely available, relatively inexpensive and well-suited to detecting soft tissue lesions near the surface of the body.
However, ultrasound can miss deep lesions, and results are highly operator-dependent. Sarcoma UK has specifically highlighted that sarcomas can be missed on ultrasound either because equipment is inadequate or because scans are mis-reported – emphasising that uncertain or borderline ultrasound results must not be accepted as reassurance. NICE guidance is explicit: if ultrasound findings are uncertain and clinical concern persists, urgent referral to a sarcoma centre should be made.
MRI – the definitive investigation
MRI is the gold standard for characterising bone and soft tissue tumours, providing detailed information about tumour location, size, depth, relationship to neurovascular structures and signal characteristics that help distinguish benign from malignant lesions before biopsy.
In the case illustrated in this article, MRI provided an unambiguous image of a 7-centimetre mass with clear margins and characteristic signal behaviour – precisely the information needed to expedite specialist referral and appropriate surgical planning.
MRI accuracy for bone tumour diagnosis is consistently higher than X-ray alone for soft tissue assessment, and superior to CT and X-ray when evaluating tumour extent and stage. Early, expert-reported MRI gives clinicians and patients the clearest possible picture – and the best possible opportunity for timely, appropriate treatment.
Under UK NICE guidelines, if a GP or clinician suspects soft tissue sarcoma – or if ultrasound results are uncertain and clinical concern persists – the patient must be referred urgently to a specialist, with the appointment to take place within 14 days.
This pathway exists because early diagnosis saves lives and limbs. Studies have shown that late diagnosis is a key driver of the UK’s historically inferior sarcoma survival rates compared with European peers, and that reducing time to diagnosis is one of the highest-impact interventions available.
The criteria for urgent referral include any unexplained lump that is increasing in size, or any situation where soft tissue sarcoma is being considered and imaging is equivocal.
As a patient, you have the right to ask your GP directly:
“Could this be a tumour? Have I had the imaging I need? Should I be referred under the two-week wait pathway?”
You should not need to ask these questions after twelve months of unexplained pain. But if you have been waiting and wondering, ask them today.
At LSRI and ScanNearMe, the principle that drives everything we do is straightforward.
We do not believe in treating assumptions. We do not believe in months of therapy directed at a diagnosis that has never been confirmed by imaging. We believe that getting the diagnosis right is the most important thing a clinician can do for a patient – and that every day of delay in reaching that diagnosis has a cost, sometimes a catastrophic one.
Dr Prashant Sankaye FRCR brings almost three decades of medical experience, specialist fellowship training in musculoskeletal and sports radiology, and a particular commitment to recognising sinister pathology – tumours, infections and inflammatory conditions – before they are mistaken for ordinary wear and tear.
This means:
- Reviewing every scan with clinical context, not just as a series of images to report in isolation.
- Recognising when findings are not what they initially appear – when a “soft tissue swelling” has features that warrant urgent further investigation.
- Communicating clearly and urgently with referring clinicians when imaging raises serious concern.
- Providing detailed, plain-English reports that patients themselves can understand and act on.
The case in this article represents a diagnostic success – the tumour was identified and appropriately reported. But it came after one year of delay. Our mission is to make that kind of delay impossible for any patient who chooses to access expert imaging through LSRI or ScanNearMe.
LSRI (London Sports and Rheumatology Imaging) is a specialist musculoskeletal imaging service built around consultant-led expertise:
- Advanced MRI and ultrasound protocols for soft tissue masses, bone lesions, sports injuries, spinal pathology and inflammatory conditions.
- Subspecialty reporting by Dr Prashant Sankaye FRCR, with experience in recognising both common and rare MSK pathology – including soft tissue and bone tumours.
- Direct integration with referring surgeons, rheumatologists, oncologists and orthopaedic specialists, so that when a serious finding is made, the right next step happens immediately.
- Based in London, with a reputation for combining accessibility and speed with the highest clinical standards.
If you have persistent limb pain, a palpable mass, or any of the red-flag features described in this article, LSRI can provide the specialist imaging and expert opinion that is the essential first step on the path to the right diagnosis and the right treatment.
Not everyone is based in London. Not everyone has easy access to a specialist MSK imaging centre. That is exactly why ScanNearMe (ScanNearMe.co.uk) exists.
ScanNearMe provides:
- UK-wide MRI access through a national network of partner imaging centres, with appointments typically available within days.
- Affordable, transparent pricing – clear costs upfront, no hidden fees, no requirement for a GP referral in most cases.
- Consultant-level reporting – scans are not processed as routine administrative tasks. Complex or concerning findings are reported with the clinical weight they deserve.
- Digital report delivery – results shared directly with you and with your chosen GP, physiotherapist, orthopaedic surgeon or oncologist, wherever in the UK they are based.
- Clinical triage – if you are not sure which scan you need, ScanNearMe’s clinical team will guide you to the right investigation based on your symptoms and history.
For any patient who has had months of unexplained pain, a palpable lump, or symptoms that have not responded to physiotherapy, ScanNearMe can provide the MRI that could answer the question your GP or physio has not yet been able to answer.
Do not wait another month. Do not book another physiotherapy session without a diagnosis. Contact ScanNearMe and get the imaging you need.
This article is written with enormous respect for all clinicians working under extraordinary pressure in primary and community care. The vast majority of persistent elbow or limb pain presentations are entirely benign – and the most likely diagnosis in any given case is still far more likely to be a mechanical or soft tissue problem than a tumour.
But the red flags exist for a reason. When pain is persistent, unexplained, nocturnal, associated with a mass or swelling, or simply not improving as expected despite appropriate treatment, the next step must be imaging – not more treatment.
NICE is clear. The MDU is clear. The oncology literature is clear. Sarcoma UK is clear.
Early imaging, interpreted by an experienced musculoskeletal radiologist, can be the difference between a curative excision of a small lesion and a major limb-salvage operation – or worse.
Please refer early. Please image before treating. Please do not let a patient spend another year with an undiagnosed tumour.
—
Dr Prashant Sankaye FRCR is a Consultant Musculoskeletal, Spine and Sports Radiologist and lead radiologist at LSRI (London Sports and Rheumatology Imaging). With almost three decades of medical experience and specialist fellowship training at Oxford University Hospitals, he has particular expertise in sports injuries, bone stress pathology, spinal imaging, rheumatological conditions and musculoskeletal tumour detection. He is the founder of ScanNearMe, a UK-wide network providing affordable, expert-reported MRI scans without long waiting lists. Dr Sankaye’s guiding principle in all clinical work is diagnose first, treat later – believing that accurate, timely diagnosis is the most important gift a doctor can give a patient.
Related Reading: Delayed Diagnosis of Stress Fractures: The Hidden Epidemic of Unexplained Pain
Related Reading: One Year of Elbow Pain, Months of Physiotherapy – and a Tumour Nobody Had Looked For
Understanding your elbow tumour diagnosis

About the Author: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
Dr Prashant Sankaye is a highly respected Consultant MSK Radiologist and the Clinical Director of London Sports & Rheumatology Imaging (LSRI). With over a decade of sub-specialty experience, he is a recognized expert in advanced diagnostic imaging (Ultrasound & 3T MRI) and precision ultrasound-guided therapeutic injections. His authoritative approach ensures patients avoid surgery where possible and receive the highest standard of orthopaedic, rheumatological, and sports medicine care.