✍️ Written by: LSRI Editorial Team
🩺 Medically Reviewed by: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
📅 Last Updated: May 3, 2026
⏱️ Read Time: 10 Minutes
Delayed diagnosis of patellar tendinopathy is far more common than most runners and active patients realise, especially when long‑standing anterior knee pain is labelled as “tendonitis” and treated for months without imaging. Two years of pain, repeated courses of non‑specific physiotherapy and no clear explanation is sadly a familiar story at LSRI, LondonSportsImaging and HarleyStreetScan.
In the case we discuss here, a patient lived with so‑called “patellar tendonitis” for almost two years. Only when a high‑quality MRI and ultrasound study were performed and reported by Dr Prashant Sankaye FRCR at LSRI – London Sports and Rheumatology Imaging did the real picture emerge: severe proximal patellar tendinopathy combined with Hoffa’s fat pad impingement, a well‑recognised but often missed source of anterior knee pain in jumping and running athletes.
At LSRI, LondonSportsImaging, HarleyStreetScan and ScanNearMe, our ethos is the same for every case: diagnose first, treat correctly, treat later – never the other way round.
What the MRI actually showed
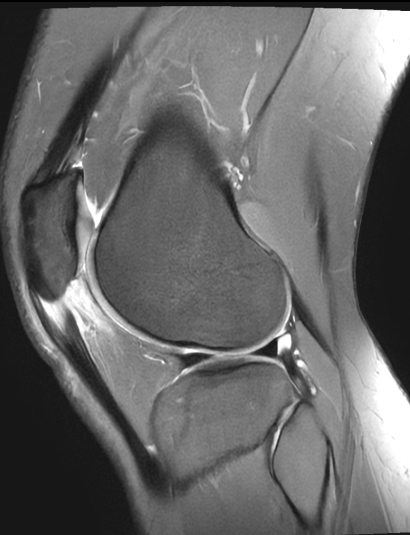
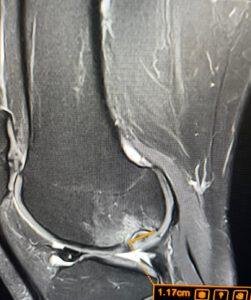
This four‑panel MRI image from LSRI shows:
- Marked thickening and signal change in the proximal patellar tendon at its attachment to the inferior pole of the patella – typical of advanced patellar tendinopathy rather than simple inflammation.
- High T2 signal and oedema in the infrapatellar (Hoffa’s) fat pad, especially deep to the patellar tendon – consistent with Hoffa’s fat pad impingement syndrome, a painful but frequently unrecognised source of anterior knee pain.

These are not minor findings. They explain exactly why two years of generic physiotherapy aimed at “knee pain” never worked: the underlying pathology had never been precisely identified, let alone specifically targeted.
At LSRI, Dr Prashant Sankaye reported these images and recommended a focused management plan including targeted loading strategies and image‑guided platelet‑rich plasma (PRP) injection into the degenerate portion of the tendon, rather than more broad, non‑diagnostic rehabilitation.
Understanding patellar tendinopathy – more than just “tendonitis”
Patellar tendinopathy (sometimes called “jumper’s knee”) is a chronic overuse injury of the patellar tendon, usually at its proximal attachment to the patella.
It is common in sports involving jumping, sprinting and change of direction, but it also affects recreational athletes and people with occupational knee loading.
Key features include:
- Localised pain at the inferior pole of the patella, typically worse with activities such as squatting, running, climbing stairs or jumping.
- Thickening, structural disorganisation and sometimes partial tearing of the tendon fibres, not just short‑lived inflammation.
- Symptoms lasting months to years if loading is not appropriately modified and if the tendon pathology is not directly addressed.
Clinical examination is essential, but studies comparing imaging modalities confirm that ultrasound and MRI provide objective evidence of tendon thickening, hypoechogenicity and neovascularity, which correlate with clinically diagnosed patellar tendinopathy and help distinguish it from other causes of anterior knee pain.
What is Hoffa’s fat pad impingement?
The infrapatellar (Hoffa’s) fat pad is a richly innervated, vascular soft tissue structure that sits behind and beneath the patellar tendon, filling much of the anterior knee joint space.
When it becomes inflamed, swollen or fibrotic, it can be pinched between the patella and femoral condyle during knee movement, causing Hoffa’s fat pad impingement syndrome.
Typical features include:
- Deep anterior knee pain felt just below or around the patella, often worse with knee extension, running downhill or prolonged standing.
- Localised tenderness either side of the patellar tendon and sometimes a subtle fullness or “catching” sensation.
- MRI findings of oedema, hypertrophy or fibrosis within the fat pad, particularly in the superolateral portion adjacent to the patellar tendon and lateral femoral condyle.
Because these symptoms can mimic patellofemoral pain, plica syndrome, bursitis or even psychosomatic pain, Hoffa’s fat pad pathology is commonly under‑diagnosed, frequently leading to a delayed diagnosis of patellar tendinopathy, and patients are often treated for “anterior knee pain” without a clear structural diagnosis.
Why delayed diagnosis of patellar tendinopathy and Hoffa’s impingement is so common
High‑quality physiotherapy is central to managing patellar tendinopathy and fat pad issues – but only when it is diagnosis‑led and load‑specific.
Typical reasons patients fail to improve after months or years of generic rehab include:
- No imaging, no diagnosis: anterior knee pain is treated as “patellofemoral pain” or “overuse” without establishing whether the primary driver is tendon, fat pad, cartilage, plica or something else.
- Non‑specific strengthening programmes: patients are given global quadriceps or gluteal exercises that do not specifically address the pathological portion of the patellar tendon or off‑load the compressed fat pad.
- Persistent aggravating loads: continuing high‑impact sport or repetitive kneeling while “doing some exercises” can prevent tendon and fat pad tissue from ever entering a healing phase.
- Failure to reassess: when symptoms do not improve within a reasonable timeframe (for example 6–12 weeks of properly dosed rehab), the diagnosis is not revisited and imaging is not requested.
Guidance for musculoskeletal imaging emphasises that non‑specific imaging requests such as “?knee pain” or “?tendon problem” should be avoided; instead, clinicians should provide clear clinical information and questions – for example “persistent anterior knee pain, query patellar tendinopathy vs Hoffa’s fat pad impingement”.
This level of precision is exactly what we encourage at LSRI, LondonSportsImaging and HarleyStreetScan, and what ScanNearMe facilitates for referrers across the UK.
The role of imaging – when and why to scan
Most patients with short‑lived anterior knee pain will improve with education, load management and basic physiotherapy, and do not need immediate imaging.
However, certain situations should strongly prompt referral for ultrasound or MRI:
- Pain persisting longer than 3–6 months despite well‑structured, diagnosis‑informed rehabilitation.
- Clear localised tenderness at the patellar tendon origin with or without a palpable thickening or nodule.
- Clinical suspicion of Hoffa’s fat pad pathology – pain just either side of the patellar tendon, exacerbated by extension or hyperextension, or ongoing swelling around the infrapatellar region.
- Previous knee surgery or trauma with new or persistent anterior knee symptoms.
- High‑level or professional athletes where precise tissue diagnosis will significantly affect return‑to‑sport decisions.
Comparative studies show that diagnostic ultrasound is highly sensitive for patellar tendinopathy, with accuracy figures around 83% and better sensitivity than MRI in some cohorts, while MRI provides excellent whole‑joint evaluation, cartilage and fat pad detail.
In practice, LSRI and LondonSportsImaging often combine both modalities, depending on the case and referrer needs.
PRP for refractory patellar tendinopathy – what does the evidence say?
For many patients, a dedicated eccentric or slow heavy‑load exercise programme, guided by an experienced physiotherapist, is enough to significantly improve symptoms and function.
However, a substantial minority develop refractory patellar tendinopathy – symptoms persisting for more than 6–12 months despite optimal rehab, load management and other conservative measures.
In this group, biologic and interventional options such as platelet‑rich plasma (PRP) injections have attracted increasing interest.
Systematic reviews and meta‑analyses show:
- PRP is a safe and biologically plausible treatment, designed to stimulate a more normal healing response in chronically degenerate tendon tissue.
- Randomised trials comparing PRP with dry needling or extracorporeal shockwave therapy (ESWT) in chronic patellar tendinopathy show similar short‑term outcomes, but some studies report better medium‑to‑long‑term VISA‑P functional scores with PRP in recalcitrant cases.
Overall, the evidence is mixed: PRP is not a magic bullet or guaranteed cure, but in carefully selected patients with accurately imaged, focal tendinopathy, it can be an important part of a comprehensive management plan.
At LSRI, LondonSportsImaging and HarleyStreetScan, Dr Prashant Sankaye’s role is to define the exact anatomical target – the precise portion of the patellar tendon showing structural degeneration – and to guide referrers towards appropriate interventional options.
At selected partner clinics, PRP injections are performed under ultrasound guidance into the abnormal segment, followed by a tightly structured rehabilitation protocol rather than generic “rest and hope”.
How LSRI, LondonSportsImaging, HarleyStreetScan and ScanNearMe work together
For patients and referrers, the pathway is deliberately simple:
- Accurate imaging at LSRI / LondonSportsImaging / HarleyStreetScan
High‑resolution MRI and diagnostic ultrasound of the knee, tailored to suspected patellar tendon and fat pad pathology. - Reports by Dr Prashant Sankaye FRCR, explicitly commenting on patellar tendon structure, Hoffa’s fat pad, cartilage, bone marrow and any additional pathology.
- UK‑wide access via ScanNearMe
For patients outside London, ScanNearMe arranges fast, affordable MRI and ultrasound appointments across the UK with consultant‑level reporting. - Reports clearly state whether significant patellar tendinopathy or Hoffa’s impingement is present and whether the findings fit the clinical picture.
- Treatment based on diagnosis, not guesswork
Referring physiotherapists, sports physicians, orthopaedic surgeons and pain specialists can then build targeted plans – from eccentric loading and taping strategies to PRP injections or, in rare refractory cases, surgical intervention.
This is the opposite of “try some exercises and see how it goes”. To avoid the delayed diagnosis of patellar tendinopathy, it is imaging‑led, diagnosis‑first care designed to save patients months or years of trial‑and‑error.
For more on the consequences of missed imaging, read our case study on delayed diagnosis of stress fractures.
When should you push for a scan?
If you recognise yourself in this story – months or years of anterior knee pain, multiple rounds of physiotherapy, no clear diagnosis – it may be time to push for imaging.
Consider asking your GP, physiotherapist or sports doctor:
- “Could this be patellar tendinopathy or Hoffa’s fat pad impingement rather than generic anterior knee pain?”
- “Have I had the right imaging to answer that question – ultrasound or MRI reported by a specialist musculoskeletal radiologist?”
- “If not, can you refer me to LSRI, LondonSportsImaging, HarleyStreetScan or arrange a ScanNearMe MRI close to where I live?”
You are not asking for unnecessary tests. You are asking for the right test for a problem that has already failed conservative care. Health‑system guidance explicitly recognises that persistent, difficult‑to‑manage musculoskeletal pain warrants targeted imaging once reasonable conservative measures have not worked.
FAQs – patellar tendon, Hoffa’s fat pad and PRP
Is all anterior knee pain patellar tendinopathy?
No. Anterior knee pain has many causes, including patellofemoral pain, bursitis, synovial plica, patellar tendinopathy, Hoffa’s fat pad impingement and others. Imaging and a good clinical exam help separate these.
How do I know if my pain is more likely patellar tendinopathy?
Pain directly at the inferior pole of the patella, worse with jumping, squatting and stairs, and sometimes with a tender “nub” in the proximal tendon are classic features. Persistent symptoms despite appropriate rehab should prompt imaging.
Can Hoffa’s fat pad impingement get better without surgery?
Yes. Many patients improve with diagnosis‑led physiotherapy, taping to unload the fat pad and activity modification, but refractory cases may need image‑guided injections or arthroscopic debridement.
Is PRP always necessary for patellar tendinopathy?
No. PRP is usually considered only after at least 3–6 months of well‑structured loading programmes and other conservative treatments have failed. Even then, it should be combined with ongoing rehabilitation rather than used in isolation.
Can ScanNearMe arrange MRI or ultrasound without a GP referral?
Yes. For most MSK problems, ScanNearMe supports self‑referral with clinical triage to ensure the correct scan is booked safely, and results are shared with your GP, physiotherapist or specialist for ongoing care.
Article written for LSRI by Dr Prashant Sankaye FRCR, Consultant Musculoskeletal, Spine & Sports Radiologist and founder of ScanNearMe.

About the Author: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
Dr Prashant Sankaye is a highly respected Consultant MSK Radiologist and the Clinical Director of London Sports & Rheumatology Imaging (LSRI). With over a decade of sub-specialty experience, he is a recognized expert in advanced diagnostic imaging (Ultrasound & 3T MRI) and precision ultrasound-guided therapeutic injections. His authoritative approach ensures patients avoid surgery where possible and receive the highest standard of orthopaedic, rheumatological, and sports medicine care.