✍️ Written by: LSRI Editorial Team
🩺 Medically Reviewed by: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
📅 Last Updated: April 6, 2026
⏱️ Read Time: 8 Minutes
Knee pain is one of the most common reasons people seek medical imaging in the UK. Whether you are a footballer, a runner, an older adult with joint pain, or someone who twisted their knee on the stairs, a knee MRI scan is often the most important diagnostic step you can take.
At London Sports and Rheumatology Imaging (LSRI London), we perform knee MRI scans every day. Patients frequently arrive with one concern above all others: they do not understand what the scan involves, what it shows, or what their results mean. This guide is written to change that.
As Consultant Radiologist at LSRI London, I — Dr Prashant Sankaye — have reported thousands of knee MRI scans. In this complete guide, I will explain what a knee MRI reveals, why it matters, how to prepare, and how to understand your results clearly and confidently.
What Is a Knee MRI Scan?
Magnetic Resonance Imaging — or MRI — uses powerful magnets and radio waves to create detailed cross-sectional images of the inside of your knee. Unlike X-rays or CT scans, MRI produces no ionising radiation and is particularly suited to imaging the knee because it captures soft tissue — ligaments, cartilage, tendons, and the meniscus — with exceptional clarity.
As with all high-technology medical devices in the UK, MRI scanners are strictly regulated by the Medicines and Healthcare products Regulatory Agency (MHRA) to ensure patient safety and technical excellence.
The knee joint is one of the most complex in the human body. It contains:
- Two menisci — the medial and lateral cartilage discs that cushion and stabilise the joint
- Four major ligaments — ACL, PCL, MCL, and LCL
- Articular cartilage — the smooth surface covering the femur, tibia, and patella
- Tendons — including the patellar tendon and quadriceps tendon
- Bone — the femur (thigh bone), tibia (shin bone), and patella
- Bursae and fluid-filled sacs — which can become inflamed
Why Has My Doctor Referred Me for a Knee MRI?
Your GP or consultant will refer you for a knee MRI when a physical examination alone cannot determine the cause of your symptoms. Our diagnostic pathways at LSRI align with the latest NICE guidelines on knee pain assessment, ensuring that every scan is clinically indicated and provides maximum diagnostic value.
Common reasons for a knee MRI referral include:
- Persistent knee pain that has not resolved with rest or physiotherapy
- Knee swelling — particularly if the joint fills with fluid repeatedly
- Locking or clicking in the knee joint
- Knee instability — the feeling that the knee might give way
- Suspected ACL or PCL tear after a sports injury
- Suspected meniscus tear after a twisting injury
- Monitoring osteoarthritis progression or severity
- Pre-surgical planning — to assess exactly what needs repair
“A knee MRI does not just tell us whether something is injured — it tells us precisely what is injured, how severely, and what the best treatment pathway is. That detail is what makes the difference between guesswork and a genuine clinical plan.”
— Dr Prashant Sankaye, Consultant Radiologist, LSRI London
Book your knee MRI at LSRI London
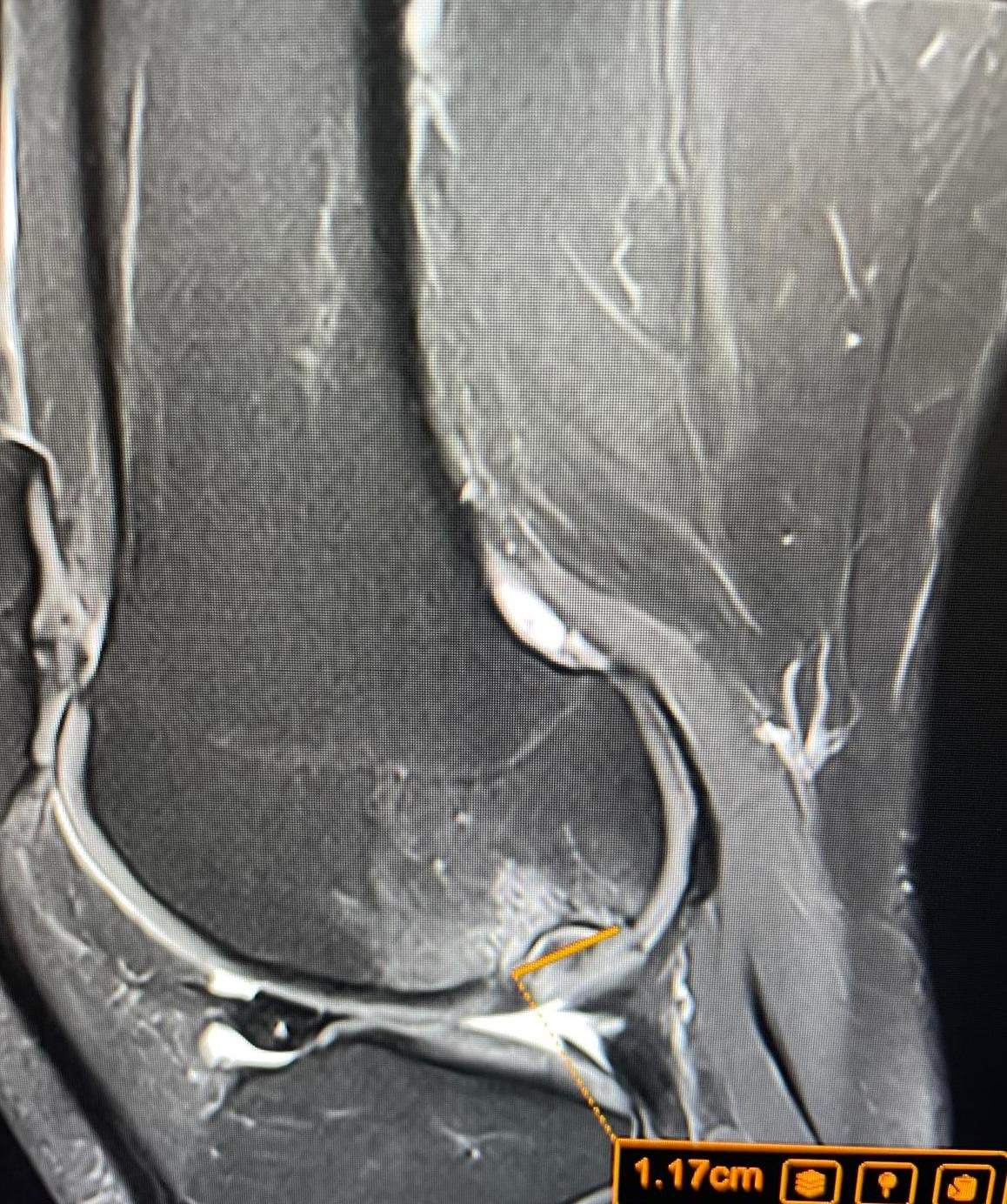
What Does a Knee MRI Actually Show?
The Meniscus — Tears, Degeneration, and Root Injuries
The meniscus is a C-shaped disc of cartilage. According to NHS data, 42.8% of patients who had a knee MRI were found to have a meniscal tear — making it the second most common finding after arthritis. MRI can detect and classify meniscal tears by type, location, and grade.
ACL and PCL — Cruciate Ligament Injuries
The ACL is one of the most commonly injured ligaments in sport. In NHS knee MRI data, 8.3% of patients were found to have an ACL tear — and over half had a combined meniscal tear alongside it.
“ACL injuries on MRI are rarely isolated findings. When I see an ACL tear, I review all surrounding structures carefully — because what looks like a simple ligament tear almost always has additional pathology that will affect the patient’s treatment and recovery.”
— Dr Prashant Sankaye, Consultant Radiologist, LSRI London
MCL and LCL — Collateral Ligament Injuries
MRI can grade collateral ligament injuries from Grade 1 (stretching) to Grade 3 (complete tear) and identify whether surgical repair or conservative management is appropriate.
Articular Cartilage — Damage, Chondral Defects, and Osteoarthritis
Osteoarthritis is the most common finding in NHS knee MRI data, present in 55.2% of patients scanned. MRI identifies chondral defects, osteochondral lesions, and cartilage thinning with precision.
Bone Bruising and Stress Fractures
X-rays often miss bone bruising entirely. Research published in the American Journal of Roentgenology found that 50% of asymptomatic adolescent footballers had bone marrow oedema detectable on MRI.
Tendons — Patellar and Quadriceps
MRI can detect tendinopathy, partial tears, and complete ruptures. Jumper’s knee (patellar tendinopathy) is a classic overuse injury in basketball, volleyball, and athletics.
Fluid, Bursae, and Baker’s Cyst
A Baker’s cyst (popliteal cyst) is frequently associated with underlying pathology such as a meniscal tear or arthritis. MRI identifies the cyst and — crucially — identifies the underlying cause.
Advanced Clinical Imaging: Behind the Pulse Sequences
At LSRI London, we use specific magnetic pulse sequences tailored to the clinical question. Proton Density (PD) sequences provide the highest resolution for the meniscus and ligaments. T2-weighted Fat Suppressed sequences are designed to detect bone marrow oedema and joint effusions — fluid that tells us the knee is in an active state of inflammation.
Special Considerations: From Young Athletes to Post-Surgical Recovery
In young athletes, we look particularly for growth plate injuries or Osgood-Schlatter disease. In older patients, we determine whether a meniscal tear is an acute injury causing current pain, or a degenerative finding that has been present for years. For post-surgical knees with metal hardware, we use Metal Artifact Reduction Sequences (MARS) to assess healing through implant distortion.
How to Prepare for Your Knee MRI at LSRI London
Preparing for a knee MRI is straightforward:
- Wear comfortable, loose-fitting clothing with no metal fastenings
- Remove all jewellery and piercings before arriving
- Inform us of any metal implants, pacemakers, or cochlear implants
- Inform us if you are pregnant or may be pregnant
- No special diet preparation is needed for a standard knee MRI
“One of the most important things patients can do before a knee MRI is simply communicate openly with our team. If you have any concerns about metal implants, claustrophobia, or previous imaging, tell us in advance. We will ensure your scan is safe, comfortable, and clinically valuable.”
— Dr Prashant Sankaye, Consultant Radiologist, LSRI London
How to Understand Your Knee MRI Scan Results
Your report will be written by Dr Prashant Sankaye or a Consultant Musculoskeletal Radiologist at LSRI London, typically available within 24 to 48 hours. The NHS provides useful context on what MRI scans involve. The Royal College of Radiologists (RCR) sets the standards our radiologists follow.
Knee MRI Scan at LSRI London — Why Choose Us?
At London Sports and Rheumatology Imaging (LSRI London), knee MRI is one of our core specialities. We adhere to the standards of the British Institute of Radiology (BIR) and the Royal College of Radiologists.
- Expert consultant reporting by Dr Prashant Sankaye
- High-field MRI technology delivering superior image quality
- Fast turnaround — results typically within 24-48 hours
- Central London location — easily accessible by tube, bus, and rail
- Self-referral accepted
Meet Dr Prashant Sankaye | Our MRI Services | Spine Services
Book Your Knee MRI at LSRI London
If you have knee pain, a suspected sports injury, or have been advised to have a knee MRI scan, LSRI London is here to help. Our team, led by Dr Prashant Sankaye, Consultant Radiologist, will ensure you receive a rapid, expert, and detailed assessment.
Book your knee MRI appointment | Contact LSRI London
Frequently Asked Questions About Knee MRI
How long does a knee MRI scan take?
A knee MRI scan at LSRI London typically takes between 30 and 45 minutes. The scan is painless and non-invasive.
Can a knee MRI detect all types of knee injury?
MRI is the gold-standard imaging tool for the soft tissues of the knee. It accurately detects meniscus tears, ACL and PCL injuries, cartilage damage, bone bruising, and tendon conditions. For complex bony detail, a CT scan may be used alongside MRI.
Do I need a referral for a knee MRI Scan at LSRI London?
LSRI London accepts both GP and consultant referrals, as well as self-referrals for private knee MRI appointments.
Is a knee MRI scan painful?
No. A knee MRI is entirely painless. There is no radiation involved. Some patients with claustrophobia find the scanner uncomfortable — please inform our team in advance so we can help.
What is the difference between a knee MRI Scan and a knee X-ray?
An X-ray shows bone clearly but cannot image soft tissues such as ligaments, cartilage, or the meniscus. MRI provides detailed images of all structures in the knee — making it far superior for diagnosing sports injuries and joint conditions.
How quickly will I get my knee MRI Scan results at LSRI London?
A formal written report from Dr Prashant Sankaye or a Consultant Radiologist is typically available within 24–48 hours of your scan.
This article has been written and medically reviewed by Dr Prashant Sankaye, Consultant Radiologist at London Sports and Rheumatology Imaging (LSRI), Central London. Last reviewed: April 2026.

About the Author: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
Dr Prashant Sankaye is a highly respected Consultant MSK Radiologist and the Clinical Director of London Sports & Rheumatology Imaging (LSRI). With over a decade of sub-specialty experience, he is a recognized expert in advanced diagnostic imaging (Ultrasound & 3T MRI) and precision ultrasound-guided therapeutic injections. His authoritative approach ensures patients avoid surgery where possible and receive the highest standard of orthopaedic, rheumatological, and sports medicine care.