✍️ Written by: LSRI Editorial Team
🩺 Medically Reviewed by: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
📅 Last Updated: March 30, 2026
⏱️ Read Time: 6 Minutes
When it comes to Sacroiliitis Diagnosis, an accurate diagnosis is the first and most critical step toward effective treatment. At LSRI London, we specialise in high-resolution imaging to ensure you receive the precise care your joints need.
Sacroiliitis — inflammation of the sacroiliac (SI) joints — is one of the most commonly misdiagnosed causes of lower back and hip pain. At LSRI, dedicated MRI diagnosis of SI joint pain is the gold standard investigation we use to distinguish sacroiliitis from lumbar disc disease and prescribe the most effective targeted treatment.
Sacroiliitis — inflammation of the sacroiliac (SI) joints — is one of the most commonly misdiagnosed causes of lower back and hip pain. At LSRI, dedicated MRI diagnosis of SI joint pain is the gold standard investigation we use to distinguish sacroiliitis from lumbar disc disease and prescribe the most effective targeted treatment.
Sacroiliitis is the inflammation of one or both of your sacroiliac joints—where your lower spine and pelvis connect. It can be surprisingly difficult to diagnose because its symptoms mimic lumbar disc issues or hip pathology.
The Challenge of Diagnosis
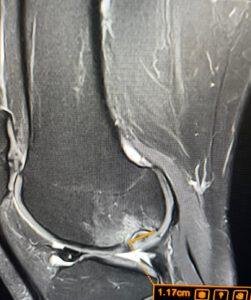
Patients often spend months being treated for “back pain” without success because the SI joint is the true source. A targeted MRI of the Sacroiliac joints is the gold standard for spotting the specific swelling (edema) that confirms this diagnosis.
Precision Treatment
If the diagnosis is confirmed, an ultrasound or CT-guided SI joint injection can provide transformative relief. By injecting directly into the narrow joint space with absolute precision, we can significantly reduce pain and improve function.
Expert Clinical Opinion: Dr Prashant Sankaye
“Sacroiliitis is frequently missed because its symptoms mimic sciatica. A dedicated SIJ MRI is the only way to avoid years of ineffective lumbar spine treatment.”
Why Sacroiliitis Is So Frequently Missed
The sacroiliac joint (SIJ) sits at the confluence of the lumbar spine and pelvis — a location that makes its pain pattern notoriously difficult to localise clinically. Patients typically report deep, unilateral buttock pain that radiates into the posterior thigh, occasionally mimicking L4/L5 or L5/S1 lumbar radiculopathy with uncanny accuracy. This clinical overlap is the primary reason why sacroiliitis is frequently misattributed to lumbar disc disease, leading to years of inappropriate spinal treatment.
The consequences are significant: patients receive repeated lumbar epidural injections, facet blocks, or even spinal fusion surgery — none of which address the actual source of pain. A dedicated SIJ MRI is the only reliable method to confirm or exclude active sacroiliitis.
Conditions That Cause Sacroiliitis
Sacroiliitis Diagnosis is not a single diagnosis — it is a manifestation of several distinct underlying pathologies:
- Ankylosing Spondylitis (AS) / Axial Spondyloarthritis (axSpA): The most clinically significant cause, characterised by bilateral inflammatory sacroiliitis that is a diagnostic hallmark of the condition. Early detection enables timely DMARD or biologic therapy to prevent spinal fusion.
- Psoriatic Arthritis: May cause asymmetric sacroiliitis in up to 30% of patients — often underdiagnosed in the absence of florid skin disease.
- Reactive Arthritis: Post-infectious inflammation that can involve the SIJ acutely.
- Degenerative Osteoarthritis of the SIJ: Common in older adults, typically unilateral, presenting after prolonged standing or walking.
- Post-Partum SIJ Dysfunction: Ligamentous laxity following childbirth can produce SIJ instability and pain indistinguishable from inflammatory sacroiliitis without imaging.
How We Diagnose Sacroiliitis at LSRI
Our SIJ imaging protocol includes:
- Dedicated SIJ MRI: Using STIR (Short TI Inversion Recovery) sequences to detect bone marrow oedema — the earliest and most sensitive marker of active inflammatory sacroiliitis, preceding structural erosions by months to years. This is the ASAS (Assessment of SpondyloArthritis international Society) recommended gold-standard imaging investigation for axSpA.
- Structural T1 Sequences: For detection of established erosions, sclerosis, and ankylosis in later-stage disease.
- Targeted Ultrasound: Used to assess posterior SIJ ligaments and guide injection placement in parallel with diagnostic confirmation.
Injection Therapy for Sacroiliitis
Once confirmed, sacroiliitis can be treated effectively with ultrasound or CT-guided SIJ injections of corticosteroid combined with local anaesthetic. In inflammatory conditions, this provides significant symptomatic relief while systemic treatment is initiated or optimised by a rheumatologist. Injection protocols are tailored to the underlying diagnosis and imaging findings — not applied uniformly.
Book a Specialist SIJ Assessment
If you have unresolved buttock, hip, or lower back pain that has not improved with lumbar spine-focused treatment, sacroiliitis should be formally excluded with a dedicated MRI. Do not spend another year treating the wrong joint. Book your specialist assessment at LSRI today.
Why Sacroiliitis Diagnosis Is So Frequently Missed
The sacroiliac joint (SIJ) sits at the confluence of the lumbar spine and pelvis — a location that makes its pain pattern notoriously difficult to localise clinically. Patients typically report deep, unilateral buttock pain that radiates into the posterior thigh, occasionally mimicking L4/L5 or L5/S1 lumbar radiculopathy with uncanny accuracy. This clinical overlap is the primary reason why sacroiliitis is frequently misattributed to lumbar disc disease, leading to years of inappropriate spinal treatment.
The consequences are significant: patients receive repeated lumbar epidural injections, facet blocks, or even spinal fusion surgery — none of which address the actual source of pain. A dedicated SIJ MRI is the only reliable method to confirm or exclude active sacroiliitis.
Conditions That Cause Sacroiliitis
Sacroiliitis is not a single diagnosis — it is a manifestation of several distinct underlying pathologies:
- Ankylosing Spondylitis (AS) / Axial Spondyloarthritis (axSpA): The most clinically significant cause, characterised by bilateral inflammatory sacroiliitis that is a diagnostic hallmark of the condition. Early detection enables timely DMARD or biologic therapy to prevent spinal fusion.
- Psoriatic Arthritis: May cause asymmetric sacroiliitis in up to 30% of patients — often underdiagnosed in the absence of florid skin disease.
- Reactive Arthritis: Post-infectious inflammation that can involve the SIJ acutely.
- Degenerative Osteoarthritis of the SIJ: Common in older adults, typically unilateral, presenting after prolonged standing or walking.
- Post-Partum SIJ Dysfunction: Ligamentous laxity following childbirth can produce SIJ instability and pain indistinguishable from inflammatory sacroiliitis without imaging.
How We Diagnose Sacroiliitis at LSRI
Our SIJ imaging protocol includes:
- Dedicated SIJ MRI: Using STIR (Short TI Inversion Recovery) sequences to detect bone marrow oedema — the earliest and most sensitive marker of active inflammatory sacroiliitis, preceding structural erosions by months to years. This is the ASAS (Assessment of SpondyloArthritis international Society) recommended gold-standard imaging investigation for axSpA.
- Structural T1 Sequences: For detection of established erosions, sclerosis, and ankylosis in later-stage disease.
- Targeted Ultrasound: Used to assess posterior SIJ ligaments and guide injection placement in parallel with diagnostic confirmation.
Injection Therapy for Sacroiliitis
Once confirmed, sacroiliitis can be treated effectively with ultrasound or CT-guided SIJ injections of corticosteroid combined with local anaesthetic. In inflammatory conditions, this provides significant symptomatic relief while systemic treatment is initiated or optimised by a rheumatologist. Injection protocols are tailored to the underlying diagnosis and imaging findings — not applied uniformly.
Book a Specialist SIJ Assessment
If you have unresolved buttock, hip, or lower back pain that has not improved with lumbar spine-focused treatment, sacroiliitis should be formally excluded with a dedicated MRI. Do not spend another year treating the wrong joint. Book your specialist assessment at LSRI today.
Sacroiliitis Diagnosis

About the Author: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
Dr Prashant Sankaye is a highly respected Consultant MSK Radiologist and the Clinical Director of London Sports & Rheumatology Imaging (LSRI). With over a decade of sub-specialty experience, he is a recognized expert in advanced diagnostic imaging (Ultrasound & 3T MRI) and precision ultrasound-guided therapeutic injections. His authoritative approach ensures patients avoid surgery where possible and receive the highest standard of orthopaedic, rheumatological, and sports medicine care.