✍️ Written by: LSRI Editorial Team
🩺 Medically Reviewed by: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
📅 Last Updated: May 4, 2026
⏱️ Read Time: 7 Minutes
Avascular necrosis hip exercises requires expert diagnosis and management.
Beyond cycling and hydrotherapy, there is a rich range of non-weight bearing exercises for avascular necrosis (AVN) that target every major muscle group around the hip. Here is the complete evidence-based breakdown organised by position and purpose.
The Core Principle
Non-weight bearing means the femoral head is not supporting body weight — so the exercise is performed lying down, seated, or suspended. The Chinese Orthopaedic Association’s guidelines specifically recommend stretching, mobility, pendulum, and low-resistance exercises without weight-bearing as the foundation of conservative AVN management.
Supine (Lying on Back) Exercises
These are the safest starting point — zero load on the femoral head.
- Heel slides — lying flat, slide heel toward buttocks and back slowly; 3 × 15 — gentle hip flexion ROM
- Supine hip abduction — slide leg outward along bed/floor surface, 3 × 15 — targets gluteus medius without compression
- Ankle pumps — flex and point foot repeatedly; reduces deep vein stasis and improves venous return from the leg — critical in AVN given the vascular compromise
- Quad sets — lying flat, press back of knee into bed tightening quad, hold 5 seconds; 3 × 10 — maintains quadriceps tone
- Straight leg raises (SLR) — lying flat, one leg bent for support, lift straight leg to ~45°, lower slowly; 3 × 10 — activates hip flexors and core without hip joint compression
- Hip abduction in sidelying — lying on side, lift top leg to 45° and lower slowly, hold 5 seconds; 3 × 10 — isolates gluteus medius
- Prone hip extension — lying face down with pillow under hips, lift straight leg upward, hold 5 seconds; 3 × 8 — activates gluteus maximus
- Supine glute bridges — feet flat, lift hips, squeeze glutes, lower slowly; 3 × 15 — the most important non-WB strengthening exercise for gluteal function
Seated Exercises
Seated exercises offload the hip significantly while allowing active muscle work and upper body conditioning.
- Seated hip flexion lifts — sitting in chair, lift knee toward chest and lower; 3 × 15 — active hip flexion without axial compression
- Seated knee extension (terminal arc) — sitting, straighten knee from 90° to full extension; 3 × 15 — activates VMO/quads
- Seated ankle dorsiflexion circles — rotate ankles in both directions; improves calf pump and reduces DVT risk
- Seated resistance band hip abduction — band around knees, push knees outward against resistance; 3 × 15 — targets glute med
- Seated upper body resistance work — bicep curls, shoulder press, lateral raises with light dumbbells; maintains overall fitness, supports weight management, and keeps cardiovascular system active without any hip load
- Chair yoga / seated stretching — seated trunk rotation, overhead reach, lateral side bends — maintains spinal mobility and reduces compensatory back pain common in AVN patients
Pendulum Exercises
Pendulum (Codman) exercises are specifically referenced in AVN guidelines and are uniquely valuable.
- Hip pendulum — standing at a table on the unaffected leg, let the affected leg hang freely and swing gently forward/back and side to side in small arcs
- The swinging motion uses gravity and momentum rather than muscle force, meaning there is virtually zero compressive load while synovial fluid is circulated and articular cartilage is nourished
- 2–3 minutes, twice daily — ideal as a morning and evening warm-up
Upper Body Cardiovascular Options
When hip pathology is severe, maintaining cardiovascular fitness requires shifting entirely to upper body:
- Arm ergometer (upper body cycle) — seated, pedalling motion with arms only — excellent non-hip cardiovascular workout
- Seated rowing machine — if hip flexion is pain-free in seated position; provides full upper body and core workout
- Resistance band seated rows and chest press — minimal hip involvement if seated with back supported
- Swimming with a pull buoy — buoy between the thighs keeps legs still, allowing upper body freestyle swimming without any hip kick — arguably the best cardiovascular option after hydrotherapy
Neuromuscular & Flexibility Exercises
These address the muscle wasting and proprioceptive deficits that develop rapidly with reduced weight-bearing.
- Electrical muscle stimulation (EMS/NMES) — applied to quadriceps and gluteals by physiotherapist; contracts muscle passively without any patient effort or joint load — particularly useful when pain inhibits active exercise
- Passive hip ROM by physiotherapist — manual mobilisation of hip through flexion, abduction, and rotation within pain-free range; maintains capsular flexibility
- Hamstring stretch (supine) — lying flat, use towel around foot to gently straighten leg toward ceiling; hold 20–30 seconds, 3 repetitions
- Hip flexor stretch (supported) — lying at edge of bed, hold one knee to chest, let other leg hang off the edge; gentle passive hip extension stretch; 20–30 seconds, 3 repetitions
Summary by Phase
| Phase | Best Non-WB Exercises |
|---|---|
| Week 1–4 | Ankle pumps, heel slides, quad sets, SLR, pendulums, EMS, seated upper body |
| Week 4–8 | Add sidelying abduction, prone extension, glute bridges, seated hip flexion lifts |
| Week 8–12 | Add arm ergometer, pull-buoy swimming, resistance band seated work, terminal arc extensions |
| 12+ weeks | Progress based on MRI review and orthopaedic/physio guidance |
The common thread across all of these is that the femoral head is never the load-bearing structure during exercise. This is not simply about pain management — it is about protecting the window of opportunity for joint preservation while maintaining the muscular infrastructure the hip joint depends on.
Dr Prashant Sankaye is a specialist musculoskeletal radiologist and CPD Approved Trainer at London Sports and Rheumatology Imaging (LSRI Ltd), CPD Provider #790052. 
Progression Principles for Non-Weight Bearing AVN Exercise
Safe progression of a non-weight bearing exercise programme for AVN follows the principle of load management — gradually increasing muscle demand while protecting the femoral head from compressive forces. Key progression markers include:
- Pain during or after exercise should remain at 3/10 or below on a numeric pain scale
- No increase in hip stiffness the morning after exercise (post-exercise soreness should settle within 24 hours)
- Serial MRI confirming stability before advancing to partially weight-bearing exercises
Combining Non-Weight Bearing Exercise with Nutritional Support
Bone healing and muscle maintenance during AVN rehabilitation benefit significantly from nutritional optimisation:
- Calcium (1000–1200mg/day) — essential for bone integrity; sources include dairy, fortified plant milks, leafy greens
- Vitamin D (at least 800–1000 IU/day) — critical for calcium absorption and bone metabolism; deficiency is extremely common in the UK
- Protein (1.2–1.6g/kg body weight/day) — supports muscle mass preservation during periods of reduced activity
- Anti-inflammatory foods — omega-3 fatty acids (oily fish, flaxseed), polyphenol-rich fruits and vegetables, and reduced processed sugar intake
The NHS nutrition guidance provides a solid foundation for patients managing long-term musculoskeletal conditions.
When to Stop Non-Weight Bearing Exercises and Seek Urgent Assessment
Immediately stop exercising and contact your clinical team if you experience:
- Sudden, severe groin pain during or after exercise — this may indicate subchondral fracture or femoral head collapse
- New acute hip locking or giving way
- Rapidly increasing pain scores that do not settle with rest
- Systemic symptoms: fever, malaise, or swelling around the hip joint
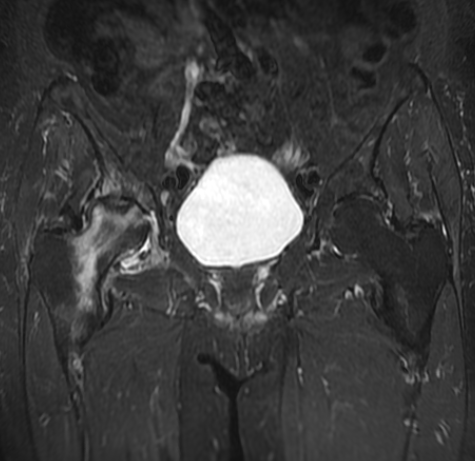
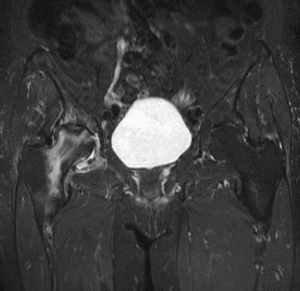
The Importance of MRI Monitoring During Rehabilitation
Exercise alone cannot reverse established AVN, but it can significantly slow disease progression and preserve quality of life while awaiting surgical decision-making. At LSRI, Dr Prashant Sankaye provides detailed serial MRI assessments, reporting on key metrics including:
- The percentage of femoral head involvement
- Presence or absence of the crescent sign (indicator of subchondral fracture risk)
- Degree of acetabular involvement
- Bone marrow oedema scoring
According to published research in the Journal of Arthroplasty, early-stage AVN managed with core decompression and physiotherapy has significantly better outcomes than later-stage surgical intervention — making early diagnosis and structured rehabilitation critical.
Contact LSRI to arrange your AVN MRI assessment or to discuss a rehabilitation monitoring programme with Dr Sankaye.
Avascular Necrosis Hip Exercises – Summary
Understanding avascular necrosis hip exercises is crucial for optimal recovery.
Essential Tips for Avascular Necrosis Hip Exercises
Practice these avascular necrosis hip exercises daily.
Gentle avascular necrosis hip exercises prevent muscle loss.
These avascular necrosis hip exercises are non-weight bearing.
Perform avascular necrosis hip exercises under guidance.
Your avascular necrosis hip exercises must be pain-free.
Mastering avascular necrosis hip exercises accelerates recovery.
Review your avascular necrosis hip exercises with a physio.
Consistent avascular necrosis hip exercises keep the joint mobile.

About the Author: Dr Prashant Sankaye, Consultant Musculoskeletal specialist and Radiologist, MBBS, MS, FCPS, MRCS, CCBST, FRCR, PGCE(Med), FHEA, PGDip Sports and Exercise Medicine
Dr Prashant Sankaye is a highly respected Consultant MSK Radiologist and the Clinical Director of London Sports & Rheumatology Imaging (LSRI). With over a decade of sub-specialty experience, he is a recognized expert in advanced diagnostic imaging (Ultrasound & 3T MRI) and precision ultrasound-guided therapeutic injections. His authoritative approach ensures patients avoid surgery where possible and receive the highest standard of orthopaedic, rheumatological, and sports medicine care.